Working closely with their system partners, three Academic Health Science Networks – Oxford, Wessex and Kent Surrey Sussex – have supported the roll out of two major programmes at pace to help keep Covid-19 patients safe and well at home.
The AHSNs were directly commissioned by NHS England and Improvement (NHSE/I) to work on two pathways relating to early identification of silent hypoxia through pulse oximetry monitoring – an approach recommended by the World Health Organisation in January 2021.
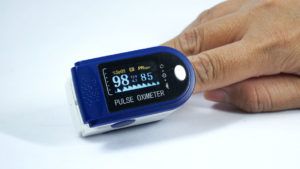
By early February around 12,000 patients in the south east had benefitted from the ‘COVID Oximetry @home’ (CO@h) service which remotely monitors patients who have, or are at risk of, Covid-19. They are given a pulse oximeter and asked to record their oxygen saturation stats. These are monitored by primary care health professionals. Should saturation levels drop below 95%, patients are contacted urgently – and admitted to hospital if appropriate.
Since January the three AHSNs have also worked closely to implement ‘COVID virtual wards’ (CVW), facilitating safe early discharge from hospital. Both initiatives have been extended nationwide. On 5 February 2021 75% of acute trusts reported having access to a COVID virtual ward.
NHSE/I wrote to all clinical commissioning groups and trusts in November 2020 to encourage the development of local CO@h projects. This followed the publication of national guidance. In January 2021 NHSE/I recommended CVWs to support earlier safe discharge of Covid-19 inpatients. CVWs reduce admissions, bed occupancy and length of stay, mitigating pressure on beds, based on evidence from early pilot sites such as this one in Reading.
There is an active discussion forum on FutureNHS (registration required) which includes our toolkits and a growing library of resources from across the country. Evaluation reports from pilot sites are also being shared on this forum. These include Slough and Reading in our region and this evaluation from University College London. Find our webinar resources here.
Tim Straughan, Director of NHS @home, said: ‘‘The AHSNs/PSCs have been absolutely fantastic to work with. They have not just supported rapid scale and spread in record time, they have created invaluable learning networks that have enabled us to continuously improve and update guidance and best practice.”
Vaughan Lewis, South East Regional Medical Director, NHS England & NHS Improvement, said: “The implementation of Covid Oximetry @home, across all six system footprints that make up the SE region, would not have been possible without the support of the three regional AHSNs. From the outset, they have collaborated as one: drawing on their combined skills and expertise, working hand-in-glove with the regional digital team – and other partners – to deliver a comprehensive service, from scratch, to achieve impressive population of this innovative model of care to promptly identify patients who need hospital admission, and to monitor those who can be safely managed at home.”
A collaboration between community leaders, GPs, NHS commissioners, researchers and the Oxford AHSN supported groups at greater risk from Covid-19. Pulse oximeters were made freely available at a foodbank, mosque and a homeless shelter linked to a GP practice. Read more in this case study.